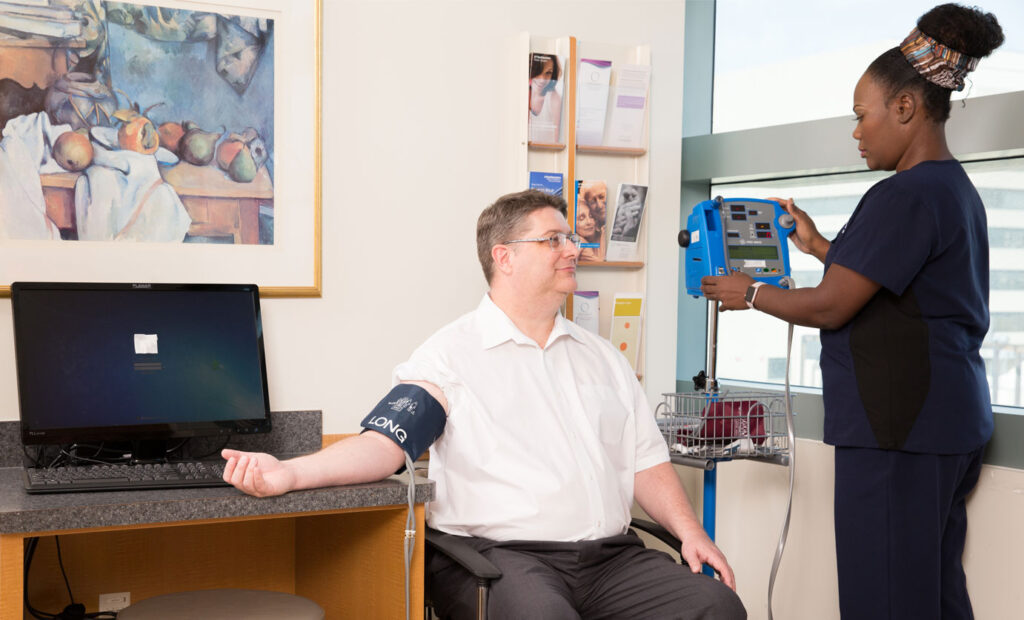
The BP Improvement Program outlines a practical, evidence-based approach to improving BP control for your patients by focusing equally on three critical areas:

Measure blood pressure accurately, every time.
Accurate measurement and recording of BP is essential to categorize level of BP, ascertain BP-related CVD risk, and guide management of high BP.

ACT rapidly to address high blood pressure readings.
Take rapid action and follow treatment protocols to bring BP under control.
PARTNER with patients, families, and communities to promote self-management and monitor progress.
Improve adherence to treatment and lifestyle changes through collaborative communication and follow-up visits.
The BP Improvement Program provides best practices, standardized processes, and useful tools designed to help you, your staff, and your patients work together to control high blood pressure. Select the strategies and tools that best fit the needs of your patients and your practice.
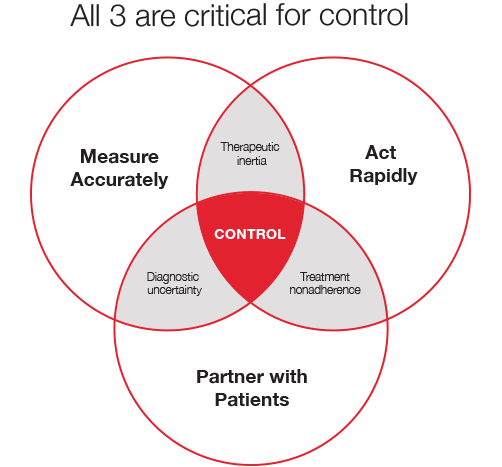
All Three Steps Are Critical for Control
Effective treatment must confront three challenges: diagnostic uncertainty—not knowing if a condition exits; therapeutic inertia—failure to initiate or escalate treatment when patients are not at goal; and treatment nonadherence—failure of patients to follow a prescribed plan, including both medication and lifestyle changes.
“A standardized treatment protocol or algorithm helps bring the team together, but also helps identify the outliers quickly, so that those who aren’t well-managed get to a higher level of care.”
Featured Resources
Aligning With Evidence-based Best Practices
Help your patients meet their BP goals by taking more accurate readings consistently; reducing therapeutic inertia to respond quickly when BP levels are high; and communicating with and encouraging patients on a regular basis.
Reduce Diagnostic Uncertainty
- Measure office BP accurately
- Confirm office BP using out-of-office BP measurements (24-hour ambulatory blood pressure monitoring or SMBP)
- Use an EHR to identify patients with undiagnosed or undertreated hypertension
Reduce Therapeutic Inertia
- Employ an evidence-based treatment protocol
- Prescribe single-pill combination therapy where appropriate
- Follow up frequently with patients
Decrease Treatment Nonadherence
- Work with patient and care team to set treatment and self-management goals
- Foster shared decision making between healthcare providers and patients
- Prioritize patients whose BP is poorly controlled, and continue to schedule follow-up visits for blood pressure measurement after medication is adjusted